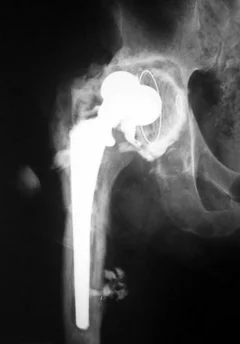

In many cases, joint replacement surgery is the last resort a sick person can rely on. But, like any operation, the operation of endoprosthetics (Joint replacement, Replacement) has its risks. These risks are higher with revision (repeated) surgical interventions.
Therefore, before deciding to undergo joint replacement surgery, you need to carefully weigh all the pros and cons of this choice.
Among European orthopedists there is an expression that arthroplasty of a joint is identical to internal amputation of this joint. And this is in a sense legitimate. After all, during endoprosthetics, quite a lot of your own bone tissue is removed, which is not restored.
Possible complications after joint replacement include:
Infectious process (paraendoprosthetic infection)
Infection in the area of the endoprosthesis (suppuration) is a serious complication. Its treatment is complex, lengthy and expensive.
The risk of developing a paraendoprosthetic infection is especially increased in patients with concomitant diseases such as rheumatoid arthritis who are taking hormonal drugs.
Infectious complications are manifested by pain, swelling, redness at the site of infection, and a sharp impairment of the supporting and motor function of the limb. Septic instability of the endoprosthesis develops. When the purulent process enters the chronic phase, a fistula is formed, from which pus is constantly or periodically released.
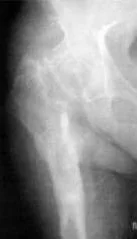
Conservative treatment is practically ineffective. Chronic postoperative osteomyelitis (purulent inflammation of the bone in the area of the endoprosthesis) is formed. In most such cases, you have to do a second operation - removal of the endoprosthesis. After this, instead of the expected appearance of a new joint, a person in this area does not even have the patient’s joint, only an “empty space”, and even a chronic purulent focus. The supporting and motor function of the limb is severely affected, and the limb is shortened. As a result, the patient remains severely disabled.
As can be seen in the above x-ray, after removal of the endoprosthesis, an “empty space” remains in the area of the former hip joint.
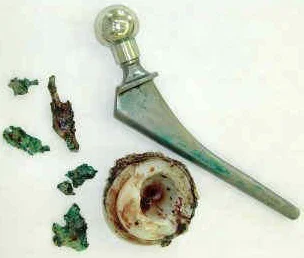
The components of the removed endoprosthesis were colored green at the points of contact with pus.

Recently, it has become possible to more successfully combat paraprosthetic infection thanks to the use of so-called articulating spacers (joint spacers). These are temporary endoprostheses made from bone cement (polymethyl methacrylate) with the addition of antibiotics. Installation of a spacer followed by its removal and replacement with a full-fledged endoprosthesis will require at least 2 more extensive operations on the joint.
With repeated attempts to replace the joint, even years after the purulent-inflammatory process has subsided, a relapse is possible.
Dislocation of the endoprosthesis
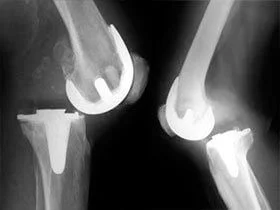
Because An artificial joint is not a complete replacement for a real joint, then its functionality is correspondingly lower. Some careless movements in the joint may cause dislocation of the endoprosthesis. As with dislocations in natural joints, it is believed that the distal component of the prosthesis is dislocated in relation to the proximal one (for example, in a hip endoprosthesis, the head of the endoprosthesis is dislocated).
Therefore, after hip replacement surgery, it is strictly not recommended to bend the leg at the hip joint more than 90°, or to rotate the leg inward.
A dislocation can also occur from a fall.
If a dislocation occurs, it is adjusted under anesthesia. After this, the leg is immobilized. After the end of the acute period, the risk of repeated dislocations always remains. If it is not possible to reduce the dislocation by closed means, an open reduction of the dislocation is performed.
Endoprosthesis fracture
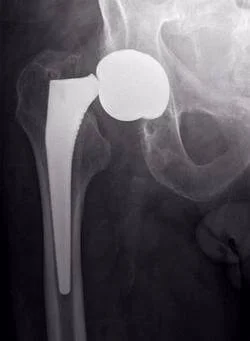
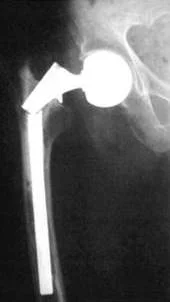
The leg or neck of the endoprosthesis may break. This is due to the so-called “fatigue” of the metal, which develops as a result of constant loads on the metal structure.
Even prostheses made from the strongest alloys are not immune to such complications.
Instability of endoprosthesis components (aseptic instability, loosening of the endoprosthesis)
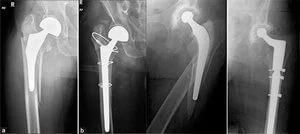
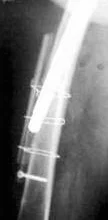
When standing or walking, a large load is placed on the endoprosthesis; micromovements occur in the connection between the bone and the endoprosthesis. As a result, the endoprosthesis becomes loose. Both the stem (femoral component) and the cup (acetabular component) of the prosthesis may become loose. The endoprosthetic leg can destroy the bone wall in which it is located - aperiprosthetic (paraprosthetic) fracture occurs.
If instability of the endoprosthesis develops, a repeat operation is required - revision endoprosthetics.
In case of a periprosthetic fracture, osteosynthesis surgery will be required, followed by long-term restriction of physical activity.
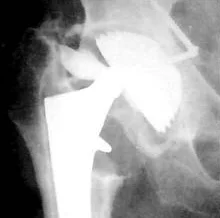
Destruction of the endoprosthesis liner
The polymer insert, which is located between the metal parts of the endoprosthesis, reduces their friction against each other during movements. It can wear out, crack, dislocate.
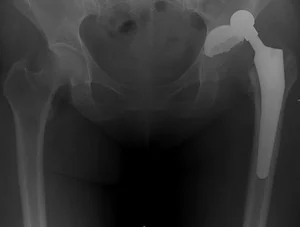
This leads to decentration of the endoprosthesis head (the presented x-ray shows a displacement of the endoprosthesis head from the center) and dysfunction of the limb.
With such a complication, repeated surgery is required to replace the liner.
Protrusion of the acetabulum
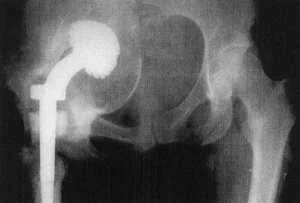
This is the introduction of the femoral component of the prosthesis (head) into the acetabulum with perforation of its wall and exit into the pelvic cavity.
This complication sharply disrupts the function of the joint (making it virtually impossible), and is also fraught with damage to the pelvic organs.
Change in the length of the operated limb
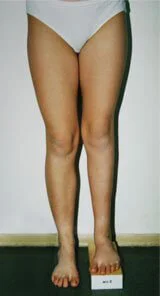
Both shortening and lengthening of the operated limb may be observed.
A similar complication can occur if the endoprosthesis is installed incorrectly. In this case, a new operation may be required.
This complication may also be caused by weakening of the periarticular muscles. In this case, it is necessary to strengthen these muscles with physical exercise.
Contracture of the prosthetic joint (limitation of movement)
Occurs during ossification (ossification) of periarticular soft tissues.
In this case, the supporting function of the limb is preserved, but the range of movements in the prosthetic joint is sharply limited.
Postoperative neuritis (traction neuropathy)
This is an inflammation of the nerves passing near the joint due to trauma (overextension or compression) during surgery.
Deep vein thrombosis of the limb
After surgery, blood clots may form in the veins of the operated limb due to decreased movements (because with low physical activity, the muscular-venous “pump” - a pump that helps the movement of blood in the veins of the lower extremities - does not work well). At the same time, blood stagnates in the veins, the blood becomes thicker, resulting in the formation of blood clots.
Therefore, early activation of the patient is recommended, as well as prophylactic administration of anticoagulants (anticoagulants).
As a result of venous thrombosis, the most dangerous complication can develop - pulmonary embolism.
Pulmonary embolism
A fatal complication is fortunately rare (up to 0.05%). The reason for this lies in the fact that after endoprosthetics, patients’ ability to form blood clots sharply increases. If such a thrombus breaks away from the wall of a blood vessel and enters the lungs with the bloodstream, the process of oxygen supply to the body is disrupted, and the patient dies. All patients after endoprosthetics are given anticoagulants, which “thin” the blood and sharply reduce the risk of such a complication.