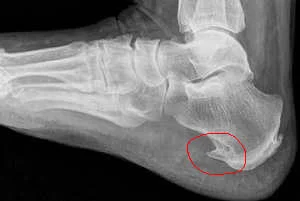
Heel spur - This is a pointed exostosis protruding from the surface of the calcaneal tubercle of the calcaneus. The spur compresses and injures the surrounding soft tissues (mucous bursae, fascia), which leads to their aseptic inflammation, accompanied by severe pain.
If the inflammation can be stopped, the spur becomes overgrown with a dense fibrous capsule, which protects the surrounding soft tissues from injury by the spur and prevents recurrence of inflammation.
Heel spurs were first described by Plettner in 1900.
Slightly more common in women over 40 years of age. It can be one- or two-sided. Radiologically, heel spurs occur, according to various studies, in 3-9% of radiographically examined patients.
Depending on the location, there are 2 types of heel spurs:
- plantar(subcalcaneal bursitis, plantar fasciitis) - on the plantar side of the calcaneal tubercle, usually on its medial process. The pain they cause is called calcanodynia. This article will look specifically at plantar heel spurs.
- dorsal - on the back side of the heel tubercle, usually develops with Achilles bursitis (inflammation of the mucous bursa under the Achilles tendon, on the back surface of the heel bone). The pain they cause is called Achillodynia.
Causes of heel spurs (etiology)
In most cases, a plantar heel spur develops as a result of flat feet. When the arch of the foot decreases, the plantar aponeurosis and short muscles of the foot, attached to the heel tubercle, are stretched. Due to constant tension, irritation and growth of the periosteum occurs, which leads to hyperplasia of bone tissue and the gradual formation of a spur.
It can also be the result of acute or chronic trauma to the heel area, overload of the feet (prolonged walking in high-heeled shoes, frequent lifting of weights, prolonged standing and long walking), gout, neurodystrophic disorders, excess body weight, some infectious diseases (especially chlamydia, gonorrhea), etc.
Diagnosis of heel spurs:
Main complaints with heel spurs
Clinical symptoms are caused not so much by the spur itself, but by inflammatory changes in the soft tissues (primarily in the mucous bursae - subcalcaneal bursitis - or in the plantar aponeurosis - plantar fasciitis).
It is interesting to note that the biggest complaints are caused by small and flat spurs. Large and sharp spurs are often asymptomatic.
The Main complaint is burning pain in the central part of the heel area, sometimes in its medial part. The pain sharply intensifies when pressing with a finger or supporting (while walking or standing) on the heel area in its central part, often closer to the medial edge. Sometimes it feels like a needle or nail has gotten into the heel.
Pain of the “starting” type, i.e. in the morning or rest period.
Symptoms and precursors of inflammation of the plantar fascia are determined bythe “singing string” test: with the patient standing, the doctor bends the thumb as much as possible (up) and jerks along the “tight string” (fascia) lengthwise and crosswise. When it becomes inflamed, the patient feels pain and withdraws the leg. The appearance of the heels may remain unchanged.
A forced body position is formed when standing, and the gait also changes. In order to walk painlessly, patients begin to walk on tiptoes or on the outer edge of the foot, trying to relieve the load on the heel.
X-ray examination for heel spurs
Typically, a heel spur is clearly visible on a lateral radiograph of the heel bone. In a direct view, the spur completely merges with the heel bone.
The spur can have a very different shape, most often spiky or wedge-shaped, its base merges with the tubercle of the heel bone, and the tip is directed forward (along the fibers of the plantar aponeurosis), sometimes in the form of a beak, slightly bent upward. In some cases, the spur has a wide base and rises above the heel bone mass with a tuberous or rough ridge.
The spur consists of a very dense, structureless substance that merges with the sclerotic surface layers of the calcaneus.
Extreme restraint is required in the clinical assessment of a spur detected by x-ray, because clinical and radiological symptoms may be unrelated to each other.
Typical pain in the heel area may be observed with a normal x-ray picture (such pain is caused by a spur that has not yet ossified). On the other hand, a spur is often discovered radiographically by chance during an examination of the foot for another reason, when there are absolutely no clinical symptoms (this is due to the presence of a dense fibrous capsule around the spur).
Heel spur treatment:
Treatment is required only in cases where the heel spur has clinical manifestations. In the absence of clinical symptoms and the presence of a spur according to X-ray data, treatment is not required.

The main treatment is conservative, aimed at relieving chronic inflammation of soft tissues and pain.
Typically, painkillers (non-steroidal anti-inflammatory drugs), ointments (warming type), physiotherapy (paraffin-ozokerite applications, magnetic therapy, ultrasound with hydrocortisone, laser therapy, shock wave therapy), blockades, and radiotherapy are prescribed.
In order to relieve the heel area, comfortable and fairly spacious shoes, orthopedic insoles, and a heel pad (silicone or just a cotton-gauze “donut”) are prescribed.
The treatment methodused inArthroclinic Akta ®, in contrast to the traditional approach, can significantly increase the chances of recovery for heel spurs. However, relapse of the disease occurs extremely rarely.
In rare, particularly severe cases, if conservative treatment is ineffective, surgical treatment may be performed - resection of the heel spur and inflamed mucous bursa.